Interview with Ms Sue Horton, CIGI Chair in Global Health Economics, Department of Economics, University of Waterloo.
The interview took place in Bangkok on March 24, 2016.
From left sitting: Sue Horton (University of Waterloo), Nemat Hajeebhoy (Alive & Thrive). From left standing: Napat Phisanbut (Unicef), Phan Thi Hong Linh (Alive & Thrive), Roger Mathisen (Alive & Thrive), and Christiane Rudert (Unicef)
The Thai Department of Health, Unicef, Alive & Thrive and the Thai Breastfeeding Center Foundation presented the latest research on breastfeeding from international medical journal The Lancet. In this interview, we talked to Sue Horton about the paper “The Cost of Not Breastfeeding in Southeast Asia”, that has uncovered some remarkable results showing why it makes economic sense for governments to promote breastfeeding.
Q: How did the study come about?
I have been working with Nemat Hajeebhoy at Alive & Thrive on the Lancet breastfeeding series, which is a big project. Alive & Thrive has been working in the region, particularly in Vietnam, to extend counseling for breastfeeding promotion and also working with the Vietnamese government to extend maternity leave, which saw very positive results on improving breastfeeding rates in Vietnam. We wanted to see how we could extend this work to other countries in the region with the view to bring about the same positive change we have seen in Vietnam. It’s an interesting challenge because not many countries have shown large and sustained increases in breastfeeding rates because it is dependent on a number of factors working together. But taking the lessons learned in Vietnam the idea was to undertake a study focusing on the cost of not breastfeeding.
Q: How would you say this study is different to previous studies?
To my knowledge, this is one of the first studies looking at the costs of not breastfeeding. There is very limited literature on economics related to breastfeeding. In fact, when we did the literature review, we only found a couple of articles on the cost effectiveness of breastfeeding, one of which I had written with colleagues some 20 years ago. But, as we began the project we started to realize that the economic consequences were actually very significant.
Q: Was that surprising?
Yes, absolutely! When we finished all the calculations for the Lancet article we went “wow!” I emailed my colleague who was leading this study as I was a bit shocked myself. Even though I had done research in this area, I never realized the enormous impact it had on cognitive development, and hence the effect on wages. The estimated economic impact certainly exceeded our hypothesis; half a percent of world GNI or $300 billion is a huge amount.
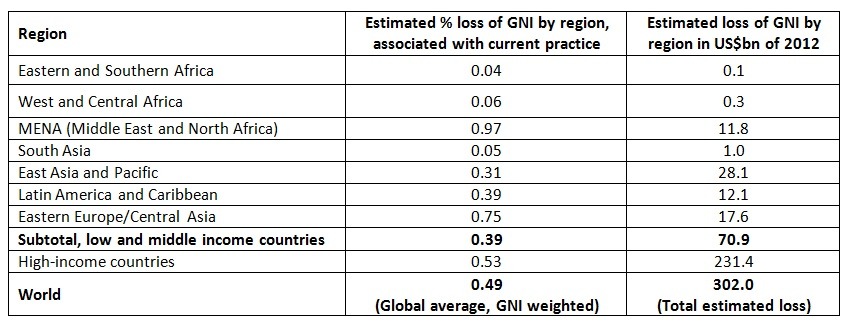
Table: Estimated economic losses (as % of GNI) associated with cognitive deficits based on current infant feeding practices, as compared to all children breastfeeding for at least 6 months
Source: Rollins, N., Bhandari N, Hajeebhoy N, Horton S, Lutter C, Martines JM, Piwoz E, Richter L, Victora C. Breastfeeding in the 21st century: Why invest, and what it will take to improve breastfeeding practices in less than a generation. Breastfeeding Series Paper 2. The Lancet 387: 491-504, 2016.
Q: How do you think this study can help improve breastfeeding practices in Thailand and other countries?
For Thailand, specifically, it highlights two gaps. Thailand is a bit unusual because it is an upper-middle income country and has a very high labor force participation rate amongst women. Women’s wages are high relative to men compared to other countries in the region. If you look at Korea, for example, it is so much different. Whilst a high participation rate certainly is positive it has a negative impact on breastfeeding, particularly since the maternity leave legislation is not very strong. Thailand only has three months maternity leave, which in part is paid by the government and in part by the employer, so there is less incentive for the women to actually take maternity leave. That is one key area to focus on. The other important issue is to strengthen legislation around the marketing code for breast milk substitutes.*
Q: So, what’s next, what else needs to be done?
This study can potentially empower other country programs by providing access to economic data that can be used as evidence. We know that breastfeeding advocates in Thailand have already outlined what needs to be changed and hopefully this study will give the government a new perspective and evoke attention from other ministries as well. The Ministry of Health needs the support of other ministries and they need evidence that matters to these other ministries. Hopefully our study is a step towards that end. There is also an opportunity for the stakeholders that came together today to take this forward. And there is more research to be done.** There was a very interesting comment made today about breast cancer. There are twice as many women in Thailand dying of breast cancer today because fewer women are breastfeeding than there are children dying of pneumonia and diarrhea because of limited breastfeeding. This raises a very interesting question. If we were to calculate the cost of breast cancer treatments, how much money could potentially be saved with the help of improvements in breastfeeding rates? Our estimate of $300 billion globally may in fact be a very conservative estimate.
*Note: On Dec 1 2015, the Thai cabinet approved a draft law. The Bill is pending review by State Council before being tabled at the National Legislative Assembly.
**Note: Work on Southeast Asia (following on from the Lancet paper) is forthcoming in Health Policy and Planning: Walters, D., S. Horton, A. Y. M. Siregar, P. Pitriyan, N. Hajeebhoy, R. Mathisen, and C. Rudert. The cost of not breastfeeding in Southeast Asia.
About the Author: Daniel Lindgren is the Founder of Rapid Asia Co., Ltd., a management consultancy firm based in Bangkok that specializes in evaluations for programs, projects, social marketing campaigns and other social development initiatives. Learn more about our work on: www.rapid-asia.com.